Reportage
Policy Course on Health System Transformation:
Private Sector Engagement for Primary Health Care-driven Integrated Health Services
The Asia Pacific Network for Health Systems Strengthening (ANHSS) at Prince of Wales Hospital, Shatin, Hong Kong on 5-7 December 2023, organized a Policy Course entitled “Private Sector Engagement for Primary Health Care-driven Integrated Healthcare”. The event provided an overview of the challenges faced in the transformation of the health system towards a primary care-led integrated healthcare system in a tax- and social insurance-funded healthcare system.
Reportage First Day
Tuesday, December 5, 2023
The Asia Pacific Network for Health Systems Strengthening (ANHSS) at Prince of Wales Hospital, Shatin, Hong Kong on 5-7 December 2023, organized the Policy Course “Private Sector Engagement for Primary Health Care-driven Integrated Healthcare”. This activity provided an overview of the challenges faced in health system transformation towards primary care-led integrated healthcare systems in tax- and social insurance-financed healthcare systems.
Welcome Message by Chairman of ANHSS
 The first day of the policy course (5/12/2023) began with remarks from Professor Laksono Trisnantoro as chairman of ANHSS. Laksono thanked the committee for their hard work in organizing the event. He also said that the previous day’s conference (4/11/2023) and today’s activities were important activities for participants to learn and implement with the main issues of equity and public private partnership..
The first day of the policy course (5/12/2023) began with remarks from Professor Laksono Trisnantoro as chairman of ANHSS. Laksono thanked the committee for their hard work in organizing the event. He also said that the previous day’s conference (4/11/2023) and today’s activities were important activities for participants to learn and implement with the main issues of equity and public private partnership..
Conceptual Framework for Engagement of the Private Sector for Health Systems Goals and Integrated Care Systems
 The opening session was followed by Professor Eng-kiong Yeoh, Director, Center for Health Systems and Policy Research, JC School of Public Health and Primary Care, Faculty of Medicine, The Chinese University of Hong Kong, Hong Kong. Mr. Yeoh’s introduction dealt with the conceptual framework for engaging the private sector in health system goals and health service integration. In addition, Yeoh also explained the program structure of the policy course. Integration of health services is explained with a conceptual framework that is formed based on the WHO Building Blocks for health systems that influence health systems and policy instruments. In this concept health financing from public, government and health services are integrated
The opening session was followed by Professor Eng-kiong Yeoh, Director, Center for Health Systems and Policy Research, JC School of Public Health and Primary Care, Faculty of Medicine, The Chinese University of Hong Kong, Hong Kong. Mr. Yeoh’s introduction dealt with the conceptual framework for engaging the private sector in health system goals and health service integration. In addition, Yeoh also explained the program structure of the policy course. Integration of health services is explained with a conceptual framework that is formed based on the WHO Building Blocks for health systems that influence health systems and policy instruments. In this concept health financing from public, government and health services are integrated
Morning plenary: Health System Transformation Provate Sector Engagement for Primary Care Led Engagement for Primary Care Led Integrated Seamless Healthcare
Prior to the inclusion of the policy course, there was a Morning Plenary session on the day by two speakers namely Dr. Libby Lee as Under Secretary for Health, Health Bureau, Hong Kong Special Administrative Region and Dr. Endang Sumiwi as Director General of Public Health, Ministry of Health, Indonesia. The three speakers discussed the Challenges for Private Sector Engagement in the Health System for Primary Care-Led Integrated Health Services.
 Lee explained that one of the challenges experienced by Hong Kong comes from health status, which is the high prevalence of chronic diseases in the elderly population. In Hong Kong, diabetes and hypertension are priority diseases that have the potential to cause twice as many complications for service costs. In addition to health status, Hong Kong also experiences challenges in health expenditure which is higher than the GDP per year. The shortage of health workers is also still experienced by Hong Kong, from the data shown the number of nurses has reached 54.6% but the availability of doctors only reached 13.3% and other health professionals only reached less than 5% for 7.3 million population. Hong Kong has taken several actions to overcome this strategy by 1) the government makes copayments with the community to get health services in public and private primary care; 2) providing incentives for family doctors; 3) providing support through district health service coordination; 4) vertical integration between family doctors with hospitals and specialists, especially for complicated diseases.
Lee explained that one of the challenges experienced by Hong Kong comes from health status, which is the high prevalence of chronic diseases in the elderly population. In Hong Kong, diabetes and hypertension are priority diseases that have the potential to cause twice as many complications for service costs. In addition to health status, Hong Kong also experiences challenges in health expenditure which is higher than the GDP per year. The shortage of health workers is also still experienced by Hong Kong, from the data shown the number of nurses has reached 54.6% but the availability of doctors only reached 13.3% and other health professionals only reached less than 5% for 7.3 million population. Hong Kong has taken several actions to overcome this strategy by 1) the government makes copayments with the community to get health services in public and private primary care; 2) providing incentives for family doctors; 3) providing support through district health service coordination; 4) vertical integration between family doctors with hospitals and specialists, especially for complicated diseases.
Primary Care Led Integrated Seamless Health Care and the Private Sector Engagement
 Different from Hong Kong, Endang explained that the primary care system in Indonesia experiences three challenges because 1) there is still a lack of integration and standardization, primary care is still centered on programs not yet life cycle needs, there is no standard in health services between health services, especially at the village level so that integration cannot run optimally; 2) gaps in availability and health facilities; 3) gaps in the ability of community health workers who lack capacity training and a less than optimal recruitment system. To overcome these challenges, Indonesia has also made efforts such as health system transformation whose main goal is to integrate primary care. This primary care integration is carried out to connect the entire network of health centers in Indonesia to the RT / RW level.
Different from Hong Kong, Endang explained that the primary care system in Indonesia experiences three challenges because 1) there is still a lack of integration and standardization, primary care is still centered on programs not yet life cycle needs, there is no standard in health services between health services, especially at the village level so that integration cannot run optimally; 2) gaps in availability and health facilities; 3) gaps in the ability of community health workers who lack capacity training and a less than optimal recruitment system. To overcome these challenges, Indonesia has also made efforts such as health system transformation whose main goal is to integrate primary care. This primary care integration is carried out to connect the entire network of health centers in Indonesia to the RT / RW level.
Panel Discussion
 Then the Morning Plenary continued with a talk show involving Professor Ying Yao Chen from China and Professor Dr. Sharifa Ezat Wan Puteh from Malaysia hosted by Professor Eng-kiong YEOH. In the talk show, Professor Wan Puteh shared that Malaysia does not have capitation funds in primary care but has subsidies from the government. In addition, primary care in Malaysia also suffers from limited health workers as experienced by several other countries. In contrast to Malaysia, the condition of primary care in China for its financial situation has sufficient capitation funds from the government. However, Chinese people tend to access more health services in hospitals and primary care does not play a strong enough role. On the issue of health workers in China, there is limited motivation to provide health services outside of the authority due to inappropriate salaries. Like Indonesia, China also has health insurance that also covers the needs of primary care. During the talk show, Yeoh also provided opportunities for participants to engage in discussions. Participants from Taiwan, Thailand and Indonesia participated to ask questions and give responses to the speaker at that time.
Then the Morning Plenary continued with a talk show involving Professor Ying Yao Chen from China and Professor Dr. Sharifa Ezat Wan Puteh from Malaysia hosted by Professor Eng-kiong YEOH. In the talk show, Professor Wan Puteh shared that Malaysia does not have capitation funds in primary care but has subsidies from the government. In addition, primary care in Malaysia also suffers from limited health workers as experienced by several other countries. In contrast to Malaysia, the condition of primary care in China for its financial situation has sufficient capitation funds from the government. However, Chinese people tend to access more health services in hospitals and primary care does not play a strong enough role. On the issue of health workers in China, there is limited motivation to provide health services outside of the authority due to inappropriate salaries. Like Indonesia, China also has health insurance that also covers the needs of primary care. During the talk show, Yeoh also provided opportunities for participants to engage in discussions. Participants from Taiwan, Thailand and Indonesia participated to ask questions and give responses to the speaker at that time.
Policy Instruments, Modalities and Mechanisms for Integrated Care
 After that, the policy course session started with a presentation from Professor Eng-kiong Yeoh who explained about the Policy Instruments, Modalities and Mechanisms for Integrated Healthcare delivered by Yeoh. Policy instruments, modalities and management is a framework aimed at integrating systems, provider organizations, and clinicians. The system is a macro level that relates to the WHO Building Blocks. Governance and leadership aspects are important to integrate providers and patients at various levels in private sector engagement. Financing is a modality to integrate the meso and micro levels. Health service aspects are important to make strategic health spending decisions in integrated services. While described at the meso level, modalities are needed to establish organizational integration, infrastructure mechanisms, functional mechanisms, professional integration, normative integration and mechanisms for clinical integration.
After that, the policy course session started with a presentation from Professor Eng-kiong Yeoh who explained about the Policy Instruments, Modalities and Mechanisms for Integrated Healthcare delivered by Yeoh. Policy instruments, modalities and management is a framework aimed at integrating systems, provider organizations, and clinicians. The system is a macro level that relates to the WHO Building Blocks. Governance and leadership aspects are important to integrate providers and patients at various levels in private sector engagement. Financing is a modality to integrate the meso and micro levels. Health service aspects are important to make strategic health spending decisions in integrated services. While described at the meso level, modalities are needed to establish organizational integration, infrastructure mechanisms, functional mechanisms, professional integration, normative integration and mechanisms for clinical integration.
Role of the Private Sector in the Asia-Pacific Region, Challenges for Integrated Health Care
 The second material on the Role of the Private Sector in the Asia Pacific Region was delivered by Professor Siripen Supakankunti as Professor, Center of Excellence in Health Economics, Faculty of Economics, Chulalongkorn University, Bangkok, Thailand. Supakankunti said that the role of the private sector can be done for health financing, provision of health services, production and distribution of medical infrastructure and medicines, education for health workers, knowledge development and investment capital. Supakankunti also explained that the role of the private sector has developed in Asia for financing, capital, investment, insurance, providers, entrepreneurs, intermediaries, governance and regulators. From this role, the private mix system has five types, namely the dominant private sector, which can complement the public sector, has high costs, is commercial, and the private sector is formed by the community.
The second material on the Role of the Private Sector in the Asia Pacific Region was delivered by Professor Siripen Supakankunti as Professor, Center of Excellence in Health Economics, Faculty of Economics, Chulalongkorn University, Bangkok, Thailand. Supakankunti said that the role of the private sector can be done for health financing, provision of health services, production and distribution of medical infrastructure and medicines, education for health workers, knowledge development and investment capital. Supakankunti also explained that the role of the private sector has developed in Asia for financing, capital, investment, insurance, providers, entrepreneurs, intermediaries, governance and regulators. From this role, the private mix system has five types, namely the dominant private sector, which can complement the public sector, has high costs, is commercial, and the private sector is formed by the community.
Policy Instrument I: Health System Governance Mechanism and Public Private Financing
 In the afternoon session of the policy course, participants received material related to policy instruments by Professor Laksono Trisnantoro as Professor of Health Policy and Management, Department of Health Policy and Management, Faculty of Medicine, Public Health and Nursing, Gadjah Mada University, Indonesia. Laksono presented material related to health system governance mechanisms and public-private financing. Like the previous material, Laksono’s material began by explaining the health system from the WHO Building Block which was linked to aspects of health financing. Entering health financing, he explained the health financing system consisting of revenue, pooling and purchasing-payment. Laksono invited participants to identify each country’s revenue from the private and public sectors. After that, the large pooling in Indonesia from BPJS Kesehatan was introduced and participants were invited to identify pooling in their own countries. After that, Laksono explained the forms of health expenditure and payment consisting of 1) resource-based allocation through the planning system; 2) payments to hospitals and health service organizations; 3) direct payments to doctors. He explained that each of these forms has problems and solutions needed, for example, capitation payments have problems of low utilization, high referral rates, low doctor attention and low community satisfaction. These problems require solutions such as UR and complaint management.
In the afternoon session of the policy course, participants received material related to policy instruments by Professor Laksono Trisnantoro as Professor of Health Policy and Management, Department of Health Policy and Management, Faculty of Medicine, Public Health and Nursing, Gadjah Mada University, Indonesia. Laksono presented material related to health system governance mechanisms and public-private financing. Like the previous material, Laksono’s material began by explaining the health system from the WHO Building Block which was linked to aspects of health financing. Entering health financing, he explained the health financing system consisting of revenue, pooling and purchasing-payment. Laksono invited participants to identify each country’s revenue from the private and public sectors. After that, the large pooling in Indonesia from BPJS Kesehatan was introduced and participants were invited to identify pooling in their own countries. After that, Laksono explained the forms of health expenditure and payment consisting of 1) resource-based allocation through the planning system; 2) payments to hospitals and health service organizations; 3) direct payments to doctors. He explained that each of these forms has problems and solutions needed, for example, capitation payments have problems of low utilization, high referral rates, low doctor attention and low community satisfaction. These problems require solutions such as UR and complaint management.
Policy Instrument II: Regulation of Private Health Sector
 After that, the afternoon session was continued by Professor Adi Utarini as Chair of the Doctoral Program, Faculty of Medicine, Public Health and Nursing, Gadjah Mada University, Indonesia. Prof. Utarini delivered material related to Private Health Sector Regulation starting from the process and mechanism. The mechanism requires six important things such as licensing, certification, accreditation, monitoring, networking and social marketing. The regulation mechanism has three types such as 1) command and control which is mandatory and has sanctions; 2) incentives which are rewards or warning sanctions in the form of money or non-money; 3) self-regulation which is providers and health professionals self-regulate the standards they want to use. Utarini said that regulation needs to focus on low costs and interventions like the pyramid and will only increase progressively if the activity fails. Within the framework of the pyramid, regulation needs to be voluntary first before it becomes mandatory and has binding controls. Dr. Utarini also shared some reflections or examples of some health issues in Indonesia.
After that, the afternoon session was continued by Professor Adi Utarini as Chair of the Doctoral Program, Faculty of Medicine, Public Health and Nursing, Gadjah Mada University, Indonesia. Prof. Utarini delivered material related to Private Health Sector Regulation starting from the process and mechanism. The mechanism requires six important things such as licensing, certification, accreditation, monitoring, networking and social marketing. The regulation mechanism has three types such as 1) command and control which is mandatory and has sanctions; 2) incentives which are rewards or warning sanctions in the form of money or non-money; 3) self-regulation which is providers and health professionals self-regulate the standards they want to use. Utarini said that regulation needs to focus on low costs and interventions like the pyramid and will only increase progressively if the activity fails. Within the framework of the pyramid, regulation needs to be voluntary first before it becomes mandatory and has binding controls. Dr. Utarini also shared some reflections or examples of some health issues in Indonesia.

After the presentation session, participants were assigned in groups to reflect on the lessons learned. On the first day of the policy course, participants were tasked with identifying challenges in integrating health services and engaging the private sector.
Reporter:
Likke Prawidya Putri (HPM UGM)
Tri Muhartini (PKMK UGM)
Reportage Day Two
Wednesday, December 6, 2023
The Asia Pacific Network for Health Systems Strengthening (ANHSS) at Prince of Wales Hospital, Shatin, Hong Kong on 5-7 December 2023, organized a Policy Course entitled “Private Sector Engagement for Primary Health Care-driven Integrated Healthcare”. The event provided an overview of the challenges faced in the transformation of the health system towards a primary care-led integrated healthcare system in a tax- and social insurance-funded healthcare system.
Private Health Sector Assessment
 The second day of the policy course (6/12/2023) began with a preview of the first meeting by Shita Dewi as Head of the Public Health Division, Center for Health Policy and Management, Faculty of Medicine, Public Health and Nursing, Gadjah Mada University, Indonesia. After that, Shita also presented material related to the Private Health Sector Assessment (PHSA). It was conveyed that PHSA needs to be carried out with specific health system objectives and is objective. The results of the PHSA are also expected to improve policy interventions and policy dialog with stakeholders to achieve national health goals. Shita provided guidelines for conducting private sector assessments through mapping. Participants were also invited to have a group discussion.
The second day of the policy course (6/12/2023) began with a preview of the first meeting by Shita Dewi as Head of the Public Health Division, Center for Health Policy and Management, Faculty of Medicine, Public Health and Nursing, Gadjah Mada University, Indonesia. After that, Shita also presented material related to the Private Health Sector Assessment (PHSA). It was conveyed that PHSA needs to be carried out with specific health system objectives and is objective. The results of the PHSA are also expected to improve policy interventions and policy dialog with stakeholders to achieve national health goals. Shita provided guidelines for conducting private sector assessments through mapping. Participants were also invited to have a group discussion.
External Quality Assurance and Accreditation: Hong Kong context
 The next speaker was Professor Chi-tim Hung as Professor of Practice in Health Services Management, JC School of Public Health and Primary Care, Faculty of Medicine, The Chinese University of Hong Kong. Professor HUNG explained the topic of hospital accreditation in Hong Kong which has developed over time. Private hospitals have their own regulations to obtain accreditation which are regulated in the Code of Practice for Private Hospitals. In Hong Kong there is also a Joint Commission International (JCI) Tracer that assists the accreditation process of private hospitals. Hong Kong has also piloted to adapt the Australian Council of Healthcare Standards (ACHS) with a four-year cycle process until self-assessment, organizational survey, self-assessment and periodic review. This hospital accreditation is considered to have a positive impact on forming teams and changing organizational culture, adding resources, improving the health system and having regular external reviews. However, the accreditation also had a negative impact on workload, difficulty in implementing new recommendations, too much paperwork, and many standards of assessment.
The next speaker was Professor Chi-tim Hung as Professor of Practice in Health Services Management, JC School of Public Health and Primary Care, Faculty of Medicine, The Chinese University of Hong Kong. Professor HUNG explained the topic of hospital accreditation in Hong Kong which has developed over time. Private hospitals have their own regulations to obtain accreditation which are regulated in the Code of Practice for Private Hospitals. In Hong Kong there is also a Joint Commission International (JCI) Tracer that assists the accreditation process of private hospitals. Hong Kong has also piloted to adapt the Australian Council of Healthcare Standards (ACHS) with a four-year cycle process until self-assessment, organizational survey, self-assessment and periodic review. This hospital accreditation is considered to have a positive impact on forming teams and changing organizational culture, adding resources, improving the health system and having regular external reviews. However, the accreditation also had a negative impact on workload, difficulty in implementing new recommendations, too much paperwork, and many standards of assessment.
External Quality Assurance and Accreditation
 In addition to Professor, there was also another speaker, Professor Adi Utarini, who discussed accreditation. Utarini explained in the perspective of regulatory quality and its purpose which has a structure of licencing, certification and accreditation. In regulating accreditation, explain the role of regulators from the government as a supervisor, accreditation agencies and the government as a provider. Utarini also shared her experience in Indonesia in implementing hospital accreditation which is regulated by the Ministry of Health. In Indonesia, the improvement of service quality has been carried out from 1988 until now which has six accreditation agencies. Currently, 2277 hospitals are in the accreditation process. Hospital accreditation in Indonesia is related to hospitals being involved in health insurance in Indonesia.
In addition to Professor, there was also another speaker, Professor Adi Utarini, who discussed accreditation. Utarini explained in the perspective of regulatory quality and its purpose which has a structure of licencing, certification and accreditation. In regulating accreditation, explain the role of regulators from the government as a supervisor, accreditation agencies and the government as a provider. Utarini also shared her experience in Indonesia in implementing hospital accreditation which is regulated by the Ministry of Health. In Indonesia, the improvement of service quality has been carried out from 1988 until now which has six accreditation agencies. Currently, 2277 hospitals are in the accreditation process. Hospital accreditation in Indonesia is related to hospitals being involved in health insurance in Indonesia.
Infrastructural Mechanism for Integrated Health Care – Global Experience
 The next speaker from Thailand was Associate Professor Chantal Herberholz as Director, Center of Excellence for Health Economics, Faculty of Economics, Chulalongkorn University. Chantal explained about the infrastructure mechanism for service integration based on global experience. PPP implementation is considered different from other policy implementations, because there is risk sharing, long-term relationships and key indicators. There are three forms of PPP, namely infrastructure based, clinical service and co-location. Of all these models, there are several influencing factors such as government willingness and commitment, legislative and regulatory environment, public capacity, private capacity, contract design, stakeholder involvement, and transparency.
The next speaker from Thailand was Associate Professor Chantal Herberholz as Director, Center of Excellence for Health Economics, Faculty of Economics, Chulalongkorn University. Chantal explained about the infrastructure mechanism for service integration based on global experience. PPP implementation is considered different from other policy implementations, because there is risk sharing, long-term relationships and key indicators. There are three forms of PPP, namely infrastructure based, clinical service and co-location. Of all these models, there are several influencing factors such as government willingness and commitment, legislative and regulatory environment, public capacity, private capacity, contract design, stakeholder involvement, and transparency.
Primary Care and Hospital PPPs in Thailand
 Then, the topic was continued by Professor Siripen Supakankunti as Professor, Center of Excellence for Health Economics, Faculty of Economics, Chulalongkorn University who explained Thailand’s experience in implementing PPP. In Thailand, PPP has been carried out in the form of co-location where there are public hospitals operated by the private sector so that services can be integrated. Many limitations of facilities and services in Thai hospitals that are cooperated are resolved by PPP. For example, there is no vehicle parking area in the hospital, so the public involves the private sector to provide the parking instructor. Dr. Supakankunti shared many experiences in Thailand in implementing PPP in the health sector especially in hospitals for the country to have good facilities and services.
Then, the topic was continued by Professor Siripen Supakankunti as Professor, Center of Excellence for Health Economics, Faculty of Economics, Chulalongkorn University who explained Thailand’s experience in implementing PPP. In Thailand, PPP has been carried out in the form of co-location where there are public hospitals operated by the private sector so that services can be integrated. Many limitations of facilities and services in Thai hospitals that are cooperated are resolved by PPP. For example, there is no vehicle parking area in the hospital, so the public involves the private sector to provide the parking instructor. Dr. Supakankunti shared many experiences in Thailand in implementing PPP in the health sector especially in hospitals for the country to have good facilities and services.
Purchasing for Integrated Seamless Health Care: Primary Care Package and Specialist and Hospital Care
 After a break, the discussion continued with another speaker, Professor Laksono Trisnantoro, discussing Strategic Health Purchasing (SHP). SHP is a new concept that is expected to make a change from passive spending to be more strategic to have good quality health services and according to standards. SHP has the characteristics of a payment system that creates incentives, selects contracts, improves health services and makes quality prices. After explaining the concept, there are three cases of Strategic Health Purchasing in the implementation of BPJS Kesehatan, TB program and performance-based financing in Indonesia. For now, Strategic Health Purchasing has not been implemented and is still very passive in its spending.
After a break, the discussion continued with another speaker, Professor Laksono Trisnantoro, discussing Strategic Health Purchasing (SHP). SHP is a new concept that is expected to make a change from passive spending to be more strategic to have good quality health services and according to standards. SHP has the characteristics of a payment system that creates incentives, selects contracts, improves health services and makes quality prices. After explaining the concept, there are three cases of Strategic Health Purchasing in the implementation of BPJS Kesehatan, TB program and performance-based financing in Indonesia. For now, Strategic Health Purchasing has not been implemented and is still very passive in its spending.
Purchasing and Organisation Mechanisms for Integrated Seamless Health Care
 The topic related to health spending was continued by the second speaker, Professor Ying Yao Chen, Deputy Dean, School of Public Health, Fudan University from China. Chen discussed the mechanism of spending and organization for health service integration. In China, health spending from OOP is very low even though the majority of people use services in hospitals more often than primary care. The availability of the number of hospitals in China itself is very large and has increased every year consisting of Public, Private Non-Profit and Private. Of the three hospitals, the number of public hospitals in China from 2017 to 2021 has decreased quite drastically in contrast to private hospitals which have increased every year. The decline in the number of public hospitals in China is due to weak support from the government such as subsidies of only 10% of health expenditure. This condition makes public hospitals in China not last long and must follow market conditions.
The topic related to health spending was continued by the second speaker, Professor Ying Yao Chen, Deputy Dean, School of Public Health, Fudan University from China. Chen discussed the mechanism of spending and organization for health service integration. In China, health spending from OOP is very low even though the majority of people use services in hospitals more often than primary care. The availability of the number of hospitals in China itself is very large and has increased every year consisting of Public, Private Non-Profit and Private. Of the three hospitals, the number of public hospitals in China from 2017 to 2021 has decreased quite drastically in contrast to private hospitals which have increased every year. The decline in the number of public hospitals in China is due to weak support from the government such as subsidies of only 10% of health expenditure. This condition makes public hospitals in China not last long and must follow market conditions.
A Policy Course on Health System Transformation: Private Sector Engagement for Primary Care Led Integrated Health Care
 In contrast to Malaysia, Professor Dr. Sharifa Ezat Wan Puteh as Professor of Public Health, Department of Community Health, National University of Malaysia explained that Malaysia does not have health insurance and still has a high Out Of Pocket. However, Malaysia has implemented Strategic Health Purchasing with the Ministry of Health as the purchaser. There are two important points that need to be done in the implementation of Strategic Health Purchasing from the Malaysian experience that can be noted, namely 1) stability of agency governance 2) utilizing a health economics approach to ensure cost-benefit. As well as using HTA in determining health benefits.
In contrast to Malaysia, Professor Dr. Sharifa Ezat Wan Puteh as Professor of Public Health, Department of Community Health, National University of Malaysia explained that Malaysia does not have health insurance and still has a high Out Of Pocket. However, Malaysia has implemented Strategic Health Purchasing with the Ministry of Health as the purchaser. There are two important points that need to be done in the implementation of Strategic Health Purchasing from the Malaysian experience that can be noted, namely 1) stability of agency governance 2) utilizing a health economics approach to ensure cost-benefit. As well as using HTA in determining health benefits.
Information and Engagement, Social Franchising
 The last speaker of the policy course today (6/12/2023) was Professor Maria Elena B. Herrera from the Adjunct Faculty of Asian Institute of Management, Makati City, Metro Manila, Philippines. Maria explained about Social Franchising, Exhortation and Information which are important parts of policy instruments. In social franchising this is done to be able to expand good policies and be replicated in different places or regions. While exhortation and information in the concept of involving the private sector need to do social marketing which is not only in the form of dissemination but is aimed at changing behavior.
The last speaker of the policy course today (6/12/2023) was Professor Maria Elena B. Herrera from the Adjunct Faculty of Asian Institute of Management, Makati City, Metro Manila, Philippines. Maria explained about Social Franchising, Exhortation and Information which are important parts of policy instruments. In social franchising this is done to be able to expand good policies and be replicated in different places or regions. While exhortation and information in the concept of involving the private sector need to do social marketing which is not only in the form of dissemination but is aimed at changing behavior.
Reporter:
Likke Prawidya Putri (HPM UGM)
Tri Muhartini (PKMK UGM)
Reportage Day Three
Thursday, December 7, 2023
Contracting in Primary Care
 The third day of the policy course (7/12/2023) began with the topic of Contracting by Prof. Laksono Trisnantoro from the Department of Health Policy and Management, FK-KMK UGM. Contracting is a mechanism of ‘purchasing’ from certain providers, for certain services, in known quantity and quality, at an agreed price, for a certain period of time. An example of contracting is the government contracting the private sector for cleaning services. Contracting has many benefits, one of which is expanding benefits for health services and extending services to rural areas.
The third day of the policy course (7/12/2023) began with the topic of Contracting by Prof. Laksono Trisnantoro from the Department of Health Policy and Management, FK-KMK UGM. Contracting is a mechanism of ‘purchasing’ from certain providers, for certain services, in known quantity and quality, at an agreed price, for a certain period of time. An example of contracting is the government contracting the private sector for cleaning services. Contracting has many benefits, one of which is expanding benefits for health services and extending services to rural areas.
Primary care and primary health care systems in rural and remote Indonesia: Exploring integrated and private sectors engagements possibilities
 Two speakers from Indonesia and Hong Kong shared about primary health care in their respective countries, and how the concept of contracting has been implemented. Dr. Mubasysyir Hasanbasri from the Department of Biostatistics, Epidemiology and Population Health, FK-KMK UGM shared a case study of contracting to expand primary care in rural and remote areas. Mubasysyir mentioned the difference between primary care and primary healthcare. Primary care is the service provided, while primary health care systems are how services are designed to meet the needs of primary care.
Two speakers from Indonesia and Hong Kong shared about primary health care in their respective countries, and how the concept of contracting has been implemented. Dr. Mubasysyir Hasanbasri from the Department of Biostatistics, Epidemiology and Population Health, FK-KMK UGM shared a case study of contracting to expand primary care in rural and remote areas. Mubasysyir mentioned the difference between primary care and primary healthcare. Primary care is the service provided, while primary health care systems are how services are designed to meet the needs of primary care.
In the context of health services in rural and remote areas in Indonesia, services are generally provided by puskesmas, government-owned health services. On the other hand, access to puskesmas by the community is generally difficult, although health services are free but the cost of transportation to the health facility itself must be paid, so services rely heavily on outreach or home visits or mobile health centers. Outreach is carried out by health workers at puskesmas, which are even limited in number (this can be seen in the picture on the left). So contracting efforts are made, for example, by paying health workers from outside these rural areas, for example Nusantara Sehat, which is carried out by the central government. Of course, this has many challenges, as mentioned by Laksono earlier. These include the limited capacity of local managers to manage the program, which makes them dependent on programs from the central government. Contracting can also lead to internal ‘jealousy’. For example, Nusantara Sehat contracts certain health workers to work in remote areas, with relatively higher incomes compared to local staff in the same position, leading to jealousy among local staff. Ideally, health services should be like those on the right, where the approach to health service delivery is multisectoral, involving the non-government sector and the community.
Dr. Mubasysyir concluded the session by suggesting what and how contracting can be applied in the future in rural and remote areas in Indonesia. Village and sub-district heads can act as executive managers of health services, in other words as purchasers. The services provided are those offered by puskesmas, individual practicing doctors, nurses, and midwives, which can include individualized health consultations, mobile clinics, vaccinations, health education and promotion, and so on.
Contracting in Primary Care: A Case Study in Hong Kong
 Furthermore, Dr. Fei-chau Pang from the Commissioner for Primary Healthcare, Primary Healthcare Office, Health Bureau, Hong Kong Special Administrative Region told about strengthening primary care in Hong Kong, a country with 7 million inhabitants and with an urban setting. Hong Kong has a dual track system, namely public and private. Public is hospital-based services. There are only 13 private hospitals, a minority of the total. Prior to the current integration efforts, the public system fees were very low, so it was preferred by the community. These low fees provided less incentive for providers to provide services related to chronic diseases, compared to acute care. As a result of health services mainly in hospitals, prevention is very low. The current focus of PPP is more on specialist care, diagnostics, ancillary, emergency, and inpatient care, and will be further strengthened towards prevention, primary care, intermediate care, and rehabilitation care. In addition, what currently applies in Hong Kong is centralized drug supplies, fixed packages, and service fees, so from the perspective of private practitioners, it is not attractive to be a service provider in collaboration with the government.
Furthermore, Dr. Fei-chau Pang from the Commissioner for Primary Healthcare, Primary Healthcare Office, Health Bureau, Hong Kong Special Administrative Region told about strengthening primary care in Hong Kong, a country with 7 million inhabitants and with an urban setting. Hong Kong has a dual track system, namely public and private. Public is hospital-based services. There are only 13 private hospitals, a minority of the total. Prior to the current integration efforts, the public system fees were very low, so it was preferred by the community. These low fees provided less incentive for providers to provide services related to chronic diseases, compared to acute care. As a result of health services mainly in hospitals, prevention is very low. The current focus of PPP is more on specialist care, diagnostics, ancillary, emergency, and inpatient care, and will be further strengthened towards prevention, primary care, intermediate care, and rehabilitation care. In addition, what currently applies in Hong Kong is centralized drug supplies, fixed packages, and service fees, so from the perspective of private practitioners, it is not attractive to be a service provider in collaboration with the government.
To improve primary health care, especially for chronic disease care, the Hong Kong government is seeking primary care integration by contracting out primary care delivery by family doctors, department of health, and district health centers, as well as hospitals.
First, there are PPP projects for certain diseases, such as cataracts. A quota is given for cataract surgeries performed by private hospitals. There are several other services that are also carried out in this regard. Second, implementing family doctor systems, where subsidies are provided for paired doctors and participants, a life course preventive care approach that includes subsidies for vaccinations and cancer screening, a community drug formulary with package prices (cheaper), a bi-directional referral scheme to the hospital for consultation with specialists, pay for performance incentives, and support for the formation of healthy living behaviors at district health centers. This last point is the third form of contracting, which involves contracting district health centers, which are non-government organizations, to provide certain services. The fourth form of contracting is to engage nurse practitioners to provide follow-up services for patients with chronic diseases who have been consulted and diagnosed by a doctor.
These are the contracting efforts made by the Hong Kong government in order to expand the coverage and quality of health services that are being carried out, and Pang closed by inviting all of us to look again at the evaluation of its implementation in the next few years.
Implementation, Monitoring and Evaluation
 The next session was about monitoring and evaluation of program implementation and achievements by 2 speakers. The first speaker was Professor Eng-Kiong Yeoh, Director of Center for Health Systems and Policy Research, JC School of Public Health and Primary Care, Faculty of Medicine, The Chinese University of Hong Kong, Hong Kong. Prof Yeoh began by describing 4 things that cause health programs to not be optimal. One of them is weak monitoring evaluation.
The next session was about monitoring and evaluation of program implementation and achievements by 2 speakers. The first speaker was Professor Eng-Kiong Yeoh, Director of Center for Health Systems and Policy Research, JC School of Public Health and Primary Care, Faculty of Medicine, The Chinese University of Hong Kong, Hong Kong. Prof Yeoh began by describing 4 things that cause health programs to not be optimal. One of them is weak monitoring evaluation.
EK gave an example of a pilot scheme for elderly healthcare voucher scheme of HK$50 for 5 units each year for those above 70 years old since 2009. In 2017, the age limit was lowered to 65 years old. The voucher is claimed by the doctor, the doctor can still charge the co-payment, but the public does not know whether the voucher has been used or not. This service design is prone to problems, as there is no incentive for doctors to claim the vouchers. Total claims have always increased since the program was launched. Most of the claims are for services provided by medical practitioners. Most of the vouchers are claimed for acute management at around 58-65%, follow-up long term conditions at around 20-30%, whereas the main problem in the elderly is chronic disease. So, the problem with the program is that it does not motivate the elderly community to follow the prevention of chronic diseases on a regular basis.
After voucher utilization, there was an increase in the proportion of people accessing public and private services, from 49% to 61%. There was no significant difference in visits to the doctor between voucher users and non-users.
The lesson here is that after the implementation of the program, an analysis of its utilization, based on community groups and others, can be carried out so that it can be seen what are the challenges and obstacles of the program, so that it can be improved and adjusted.
Furthermore, EK explained that in program implementation, it is necessary to have an implementation plan, an evidence-based program implementation methodology, and develop clear criteria and methods for monitoring and evaluating the intervention and implementation of the program.
One of the advantages of applying a scientific framework is that it can identify factors that can contribute to program success. One example provided by EK is the Consolidated Framework for Implementation Research (CFIR), which looks at a program implementation from external, internal, individual aspects, the implementation process, and the characteristics of the program itself. CFIR can help identify barriers to program implementation, and choose what strategies can be taken to overcome these barriers.
n the implementation process, it is important to reach consensus from stakeholders, one of which can be done with a Delphi study.
EK concludes with how the integration of health services at the micro, meso and macro levels is linked using CFIR principles.
 After the first speaker explained the scientific evidence behind monitoring and evaluation, the second speaker, Professor Maria Elena B. Herrera, Adjunct Faculty of Asian Institute of Management, Makati City, Metro Manila, Philippines, presented the application or practice of program implementation, monitoring and evaluation.
After the first speaker explained the scientific evidence behind monitoring and evaluation, the second speaker, Professor Maria Elena B. Herrera, Adjunct Faculty of Asian Institute of Management, Makati City, Metro Manila, Philippines, presented the application or practice of program implementation, monitoring and evaluation.
In terms of monitoring, it is important to remember that health services are a system, and it is important to identify the root causes of problems in the program. “By conducting a good and thorough assessment, it can determine a good implementation plan for health service integration,” continued Prof. Herrera.
The key to monitoring and evaluation is understanding the systematic relationship between one aspect and another. Herrera emphasized that every strategy or policy has hypotheses. “If we do this, this will happen, under specific assumptions”. In conducting monitoring and evaluation, it is also important to use a people-centered approach. To achieve this, Herrera continued,
“Designing monitoring and evaluation for integration efforts is an iterative and feedback-driven process”. It requires a lot of discussion to come up with innovative ideas. Pilot studies play an important role in developing monitoring and evaluation. The pilot study and the overall effort can result in what indicators need to be observed, e.g. is this indicator actionable and measurable?.
Discussion of Challenges in Primary Health Care-Led Integrated Healthcare Systems and Private Sector Engagement in a Country Context
In this last session, each group presented the results of their discussion about the challenges in health service integration. The first group presented challenges from Indonesia. The first challenge is that some national programs have tried to involve the private sector in health services, but there are still minimal incentives for the private sector. However, some programs do not have policies for private sector involvement. The proposed strategies are first to provide incentives to increase private sector involvement, mapping which health services are prioritized and can be contracted out to the private sector.
The next group presented the challenges of private sector integration in Hong Kong. The first challenge is the increasing proportion of elderly people, the inequality of service costs in the public and private sectors, and the lack of awareness of personal health care. The public sector is usually preferred because it is cheaper and of good quality, but waiting times are long, while the private sector is more fragmented but waiting times are short. Similar to Indonesia, limited funding is a major challenge in terms of private sector integration. Thus, several aspects are recommended. First, in addition to the existing schemes of elderly healthcare voucher scheme, chronic disease co-care scheme, district health center, general outpatient clinic PPP, cancer screening, a change in health financing is recommended.
Another developed country is Singapore. With life expectancy exceeding 80 years, Singapore has a high proportion of elderly population. The health financing system has MediSave, MediFund, MediShield Life, and government subsidies, plus additional schemes such as Healthier SG and CHAS for access to private GPs. Public clinics cover 20% of total care but 45% of services are for chronic diseases, so there are long waiting times. The main challenge is to improve chronic disease services, which are mostly provided by government facilities. Some of the strategies proposed are social marketing, community engagement and regular evaluation. There needs to be attractive pricing for the private sector, subsidies in publicly owned polyclinics, expanding the gatekeeping role for GPs (usually patients do not need to go to a GP to get subsidized services), multi-sectoral collaboration. One example is collaborating with the private sector in designing technology-enabled self-management to monitor risk factors and morbidity of non-communicable diseases, organizing teleconsultation for gatekeeping and monitoring of chronic diseases.
In China, there is primary care in the form of community health centers, secondary care in the form of community hospitals, and tertiary care in the form of hospitals. From the analysis of group 4, it was found that the quality of health services in the private sector is actually less good than the public sector. Another gap is the lack of health promotion in integrated health services. To integrate health promotion, we will do organizational integration with strategic alliance, involving primary care practitioner-led. In addition to organizational integration, group 4 recommends professional integration in implementing health screening and counseling. Regarding contracting, what will be done is to contract doctors and nurses to conduct capacity building and training at the village level for community health centers.
The last presentation from Taiwan (Siwei Huang) explained that the National Health Insurance (NHI) in Taiwan is in the form of single payer which has covered 99% of the population. The payment process is a global budget payment system with a fee for service payment method. The private sector owns more than 83% of hospitals and 98% of clinics. There are medical records stored in the Media Cloud through the NHI program. Public satisfaction with the NHI program is over 90%. However, the NHI system has been in deficit since 2017, health workers are overworked, and life expectancy is 79 years, the lowest in a decade. The existence of global budget payments (prospective) with (retrospective) is confusing and poses a risk of competition issues and lack of coordination between healthcare providers. The proposed strategy is to utilize different payment mechanisms e.g. DRGs, capitation. In terms of payment methods, regulatory changes are proposed to strengthen the role of gatekeepers and improve the referral system, adjusting copayment values for different levels of health facilities. Regarding health worker burnout, the proposed strategy is a scheme to incentivize health workers. The strategy for the last challenge, which is unintegrated data, the proposed solution is to strengthen the NHI database. The last strategy proposed is the adoption of external quality assurance and accreditation and database integration for monitoring and evaluation. Some inputs from the speakers included how the recommendations could be more specific, especially in terms of how to initiate the strategies. It is also necessary to consider other strategies in addition to infrastructure PPPs such as co-location.
Reporter:
Likke Prawidya Putri (HPM UGM)
Tri Muhartini (PKMK UGM)
Reportage Hospital Tour Prince of Wales Hong Kong
December 8, 2023
 After the participants participated in a series of knowledge events and policy courses on December 4-7, 2023. The Asia Pacific Network for Health Systems Strengthening (ANHSS) committee together with the Hong Kong Hospital authorities and the Prince of Wales Hospital provided a hospital tour for participants on December 8, 2023. The hospital tour was hosted by Professor Chin-tim Hung and Dr. Leung Kwan Wa Maria and other health workers.
After the participants participated in a series of knowledge events and policy courses on December 4-7, 2023. The Asia Pacific Network for Health Systems Strengthening (ANHSS) committee together with the Hong Kong Hospital authorities and the Prince of Wales Hospital provided a hospital tour for participants on December 8, 2023. The hospital tour was hosted by Professor Chin-tim Hung and Dr. Leung Kwan Wa Maria and other health workers.
 The hospital tour started with an introduction to part of the building around Shaw Auditorium. Dr. Hung explained that the hospital has 1600 beds and there is a new building under construction that will expand to around 2400 beds. The new hospital is expected to be operational by 2027 with assistance from the private sector.
The hospital tour started with an introduction to part of the building around Shaw Auditorium. Dr. Hung explained that the hospital has 1600 beds and there is a new building under construction that will expand to around 2400 beds. The new hospital is expected to be operational by 2027 with assistance from the private sector.
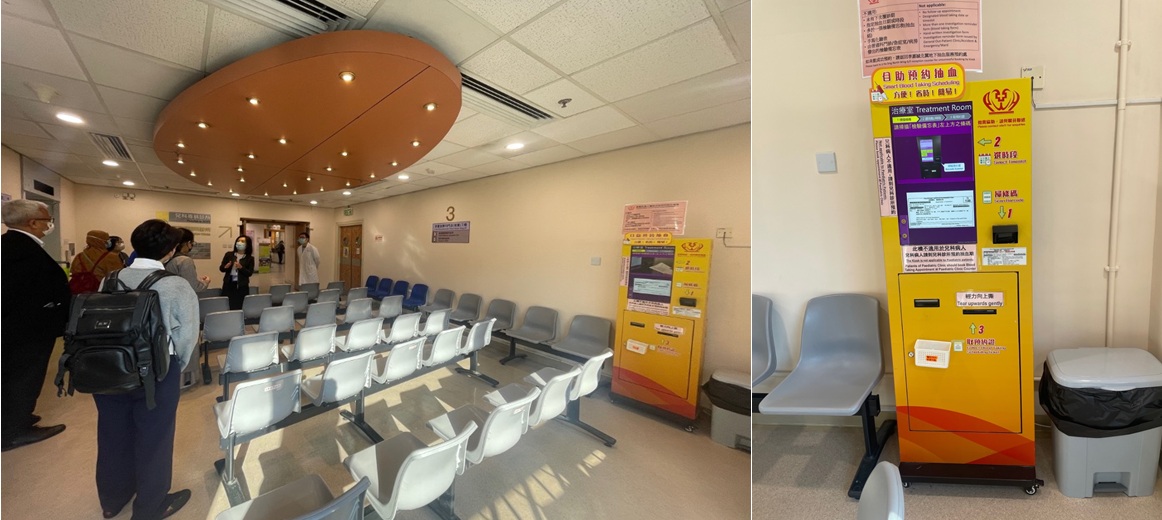
The second location of the hospital tour was the Family Medicine Department guided by Dr. Leung Kwan Wa Maria. Maria showed us where Family Medicine services provide primary health care to the community through general outpatient clinics and Family Medicine Specialist Clinics. Their main target patients are the elderly, low-income groups, and people with chronic diseases. In the Family Medicine Department, they have a Self-Scheduling machine for Blood Draws before entering the waiting room. Through the machine, patients can set their own schedule and location for blood test. In addition, Maria also explained that the Hospital Authority in Hong Kong also has an integrated medical record so that patients who move health facilities do not need to re-register and bring proof of previous medical history, all health facilities in Hong Kong can access patient data based on population numbers.
 The Department of Family Medicine has a network of 10 General Outpatients Clinics and 3 Family Medicine Specialist Clinics (FMSC). From the presentation by Dr. Lee Man Kei, GOPC has been visited by 469,260 patients and FMSC has been visited by 43,157 patients. Patients from GOPC are related to episodic disease cases and require regular follow-up for chronic diseases. While patients at FMSC are mostly referrals for treatment of referrals from other Specialist Clinics.
The Department of Family Medicine has a network of 10 General Outpatients Clinics and 3 Family Medicine Specialist Clinics (FMSC). From the presentation by Dr. Lee Man Kei, GOPC has been visited by 469,260 patients and FMSC has been visited by 43,157 patients. Patients from GOPC are related to episodic disease cases and require regular follow-up for chronic diseases. While patients at FMSC are mostly referrals for treatment of referrals from other Specialist Clinics.
Not only did participants have the opportunity to get to know Prince of Wales Hospital, Dr. Maria also prepared several presentation sessions. The first session discussed the public and private primary care system in Hong Kong. The public role is through the Hong Kong Health Bureau which is implemented by the Department of Health to manage public health. Meanwhile, the private sector provides primary care through independent practices and independent Chinese medicine. Primary care in Hong Kong is closely linked to the Hospital Authority which manages secondary care consisting of hospitals, general outpatient clinics, specialists, and Chinese medicine. Under the Hospital Authority in Hong Kong, there are 7 clusters with 74 general outpatient clinics with a total of 5.2 million patient visits. The management of Hong Kong’s primary and secondary services still faces challenges such as Public Hospitals provide care for 90% of inpatients.
Other challenges include outpatient and inpatient services having many patients with chronic diseases and long waiting times for new cases at Specialist Clinic Outpatients. These challenges are addressed by Hong Kong attempting to implement an integration model between primary care, secondary care, patient, private, patient, community, and government programs. In the integration model, each element is linked to Hong Kong government programs which are all interrelated. Such as for primary care (GOPC) and hospitals to connect requires a relationship with FMSC, and for GOPC to connect with patients requires a relationship with the District Health Center (DHC). Then for primary services, involving the private sector requires PPP and for involving NGOs, primary services can use Smart Hub. Hong Kong’s integration system of each service and target group has a medium that connects it. The main one is the DHC which Hong Kong has recently implemented with the role of connecting GOPC and Family Doctor. In addition, the DHC conducts promotion, prevention, screening, and case management. The results of DHC screening findings are linked to GPOC and Family Doctor as gatekeepers for secondary health care follow-up.

From the exposure in the hospital tour, there is the involvement of NGOs in primary care which is another important point. In Hong Kong, the government provides support to NGOs to provide services to the community. This financial support is followed up by the Department of Health and the Hospital Authority to collaborate with NGOs through the SMART Hub program. In the program, NGOs located in remote areas of Hong Kong are expected to help fulfill the primary care of the community with Telemedicine. This service fulfillment is carried out by NGOs obtaining smart medical devices, assisting the implementation of teleconsultations between doctors and patients in remote areas. With SMART Hub, local NGOs become an extension of primary care in Hong Kong with a recruitment process, conducting patient empowerment programs, tele-consultation, drug delivery and counseling, monthly visits and face-to-face meetings per year.
 The last presentation session of the Hospital Tour was on Integration between private and secondary care for Chronic Diseases in Care Co-Piloting (CDCC). The policy has been set by the Hong Kong government in 2022 with subsidies for people who get early diagnosis in private sector services. The CDCC is being piloted to provide screening, monitoring and intervention in chronic diseases and complications. The CDCC utilizes the role of Family Doctor to provide services to all communities so that the service process is: screening of people aged 45 years and above at DHC – DHC connects patients to a Family Doctor – provides subsidized care – provides long-term care when patients have a diagnosis of high blood pressure/high blood sugar. Patients who receive CDCC have other criteria, such as not only being over 45 years old but also having no known medical history or condition, being registered with DHC and agreeing to have their data shared with the EHRSS program.
The last presentation session of the Hospital Tour was on Integration between private and secondary care for Chronic Diseases in Care Co-Piloting (CDCC). The policy has been set by the Hong Kong government in 2022 with subsidies for people who get early diagnosis in private sector services. The CDCC is being piloted to provide screening, monitoring and intervention in chronic diseases and complications. The CDCC utilizes the role of Family Doctor to provide services to all communities so that the service process is: screening of people aged 45 years and above at DHC – DHC connects patients to a Family Doctor – provides subsidized care – provides long-term care when patients have a diagnosis of high blood pressure/high blood sugar. Patients who receive CDCC have other criteria, such as not only being over 45 years old but also having no known medical history or condition, being registered with DHC and agreeing to have their data shared with the EHRSS program.
From the hospital tour, learning about the integration of health services is an important line that there is a clear and specific division of roles between stakeholders, there is data sharing between health sector stakeholders that is transparent and accountable and there is sufficient resource support to be able to involve parties outside the government authority in the health service system.
Reporter: Tri Muhartini

